Author: Samay Inampudi
Mentor: Dr. Emma Sarro (Dominican College, Blauvelt, New York)
Oswego East High School
September 1, 2021
Abstract
Parkinson’s Disease is a well-known and potentially life-crippling disease which puts thousands in hardship per year. This study aims to uncover the geographical/ethnic influence on this in relation to the Gut-brain axis which is the bidirectional pathway from the gut to the brain. Studies have been done on parts of this question, but never the whole issue. Typically, researchers focus on the Gut-Brain axis or ethnicity/geographical location in relation to Parkinson’s disease. But, rarely a combination of these. This manuscript allows for the scientific community to understand specific triggers which may quicken or even cause the appearance of Parkinson’s Disease in patients worldwide. To understand the treatment, we must understand the causes. This study is a systematic review of several articles which answer parts of the whole question. Several keywords were searched and examined to create an organized, detailed review. Through this, we have found a correlation between the epidemiology of ethnic/geographic backgrounds and the Gut-brain axis in relation to Parkinson’s disease. This is vital for understanding due to the lack of knowledge in the field of how Parkinson’s is caused or progressed.
Introduction
The brain is a complex organ that underlies all of our thoughts and behaviors. Unfortunately, there are a number of complex issues such as those that slowly destroy its tissues, i.e., neurodegenerative diseases, which interfere with its ability to function. Neurodegenerative diseases typically involve the progressive death or breaking down of a part of the brain, therefore, they are consequently one of the hardest to cure and treat. Due to this, many research efforts focus on ways to slow down these neurodegenerative diseases. Of all neurodegenerative diseases, Parkinson’s Disease (PD) is one of the most common.
Parkinson’s Disease is a neurodegenerative disease that affects the movement of the patient as well as is known to cause apathy, depression, constipation, sleep issues, cognitive impairment, etc (Parkinson’s Disease, 2020). This disease targets the central nervous system (CNS), and specifically, the dopamine-producing (“dopaminergic”) neurons in an area of the brain called substantia nigra, a small nucleus in the brainstem (What is Parkinson’s?, 2021). The death of these dopamine-releasing neurons causes the symptoms of Parkinson’s such as tremors, stiffness, trouble walking, etc, due to its impact on the targets of these neurons, the Basal Ganglia. Typically in the earlier stages of Parkinson’s, a patient’s face may show little or no expressions, their arms may not swing when walking, their speech might become slurred, and several other movement issues will arise as time passes (Parkinson’s Disease, 2020). Although Parkinson’s is one of the most studied neurodegenerative diseases, the causes and ways to successfully treat the disease are still not known. Scientists have determined that there could be a genetic link to the development of the disease, and in fact, have isolated a specific gene that might increase one’s chances of developing PD. With this, there are potentially many environmental triggers (i.e. toxins, climate, etc) that can act on this genetic combination, but again this is not well established. Furthermore, scientists have begun to study some of the physical characteristics of the neurodegeneration associated with the disease. Specifically, patients with PD have a substantial amount of Lewy bodies in the brain, and in these structures, scientists believe an important protein is located. This natural and plentiful protein is called alpha-synuclein (a-synuclein), and is found in all Lewy bodies in a clumped form that cells are unable to break down (Parkinson’s Disease, 2020). Currently, this is a very popular topic among scientists researching PD. This disease is extremely difficult to live with and only gets worse as time passes, therefore, it is vital to understand the potential causes and potential risk factors.
Although food may seem like an unlikely origin for a Neurodegenerative disease, the correlation between the stomach/intestines or the gut and the brain may be deeper than initially thought. There is a biological pathway referred to as the Gut-Brain Axis (GBA) which shows a possible relationship between gut health (microbiome, food intake, etc.) and brain health (diseases, cognition, etc.). The pathway is a bidirectional network that can communicate through neural, endocrine, immune, and humoral links. It is vital to explore these links due to the huge impact it may have in the future. One area that has received an increasing amount of attention in its relation to the human condition is the microbiome located within the human body. This microbiome is the presence of a community that consists of microorganisms in a specific habitat. This microbiome’s impacts are largely unexplored, but they are known to help with metabolism, immunity, etc. In a study done by Romano et al. they concluded that there were consistent differences between PD patients and control patient’s gut microbiome (Romano et al., 2021). Although there was slight variation between trials they accounted for the variability derived by the sampling cohorts to show there was consistency in the alteration of the microbiome between the trials.
One such organism in this microbiome that has been demonstrated to exist in lower levels in PD patients compared to control patients is Lactobacilli. These bacteria are extremely vital to our gut health and have been observed in our gut from the first instances of gut microbiota composition studies. These organisms are commonly found in our digestive and urinary tracts. They reside here to assist with the breakdown of foods as well as the absorption of their nutrients. Additionally, they aid the immune system in fighting pathogens from harming the body (LACTOBACILLUS: Overview, Uses, side Effects, precautions, Interactions, dosing and reviews 2020).
This organism is vital for our health and could be a factor in the risk of developing PD. Typically, one can eat foods containing this bacterium such as yogurt, but probiotics naturally found in food such as onions, garlic, and bananas can stimulate and foster the growth of this bacteria as well as other good bacteria (GMFH Editing Team, 2020). Typically, we see these foods eaten more in eastern countries than western countries which could be a possible link to the increased and decreased appearance of PD which will be discussed in the results this presents as a possible link to microbiome-associated PD occurrences.
Thus, this paper will examine the evidence to explore a relationship between geographic patterns of PD prevalence and the associated microbiome patterns. The extensive research done thus far enables us to predict that areas with a higher incidence of Parkinson’s, such as the western world (ie: America, South America, etc), are associated with a microbiome content containing lower levels of Lactobacillales, along with others to be discussed below in further detail, as well as lower gut microbiota diversity. These factors are discussed as possible predictive factors for an increased risk of developing Parkinson’s Disease.
Methods
As a systematic review, the methods were largely based on extensive literature search and assessment. Searches were completed primarily throughout the month of July, using search engines: ”Google Scholar”, “PubMed”, and “Britannica”. Key terms used included, but not always simultaneously, were: “Parkinson’s disease” [AND/OR] “gut” [AND/OR] “microbiome” [AND/OR] “microbiome diversity” [AND/OR] “Lactobacillus” [AND/OR] “Western gut microbiota” [AND/OR] “Eastern gut microbiota” [AND/OR] “Parkinson’s epidemiology” [AND/OR] “Gut-brain axis”. Articles were then screened to determine if they contained relevant information for this study. If found to be relevant or useful, articles were contained within topic folders for deeper analysis.
Inclusion factors: We included studies that compared the composition of the gut microbiota between PD patients and control populations. We also included studies that examined the epidemiology of PD worldwide as well as within specific countries or continents. Slight variations in methodology were accounted for in this study. Additionally, all included studies were published within the last 20 years (2001-2021). Along with this, all studies using data must have a 95% confidence interval.
Results
Worldwide prevalence of Parkinson’s Disease
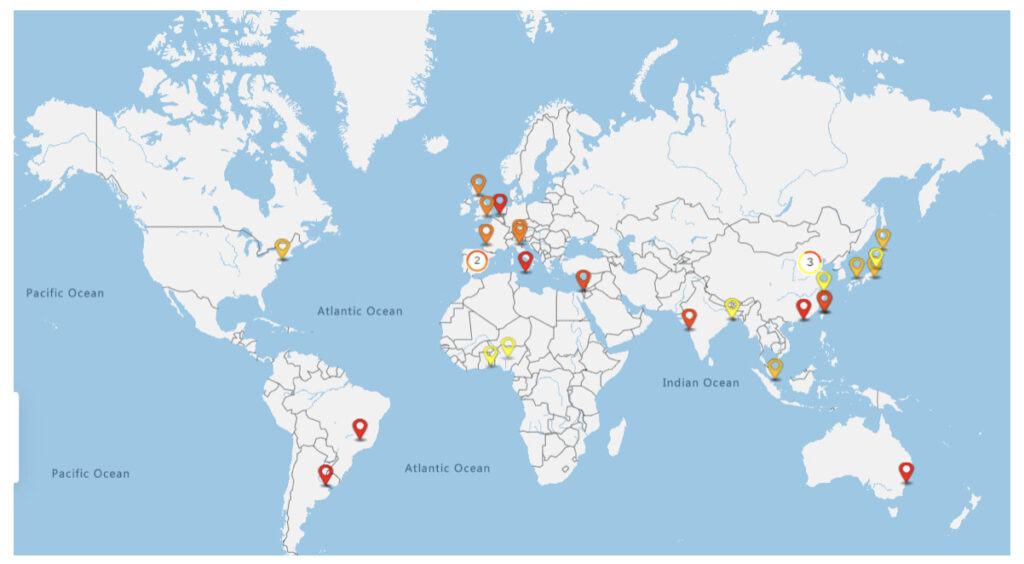
The mechanisms underlying Parkinson’s Disease are not yet fully understood, however, there seems to be a correlation between PD and geographical location. The pattern of this epidemiology suggests that there are likely several environmental factors that influence the occurrence of this disease. In a study done by Abbas and others (2017), a door-to-door study was conducted which took data from populations worldwide, many of the eastern countries had significantly less crude prevalence rates (per 100,000) than many of the western countries. For example, Bambuí, Brazil (2006) had a crude prevalence rate of about 3,330 per 100,000 people (>64 years) compared to Beijing, Xian, Shanghai, China (2005) with a prevalence rate of about 1,700 (>65 years). This study concluded that PD incidence is also lower in Asian countries compared to Western ones; although it should be noted that data was limited for Asian studies. Other studies on different ethnic populations have reported a lower PD occurrence in Eastern (Asia/Africa) than Western countries (Caucasians, Hispanics, Latinos) (Abbas et al., 2017). While this could suggest a genetic influence on the risk of developing PD, the higher rate of occurrence of PD among ethnic groups in America (African Americans and Japanese Americans) compared to similar populations in their native country, suggest an environmental role in PD. This draws concern as to what differs between these countries and several things may come to mind. Such differences could include culture, race, food, climate, flora, and fauna, etc. Specifically, with regards to food, there could be differences in the availability of processed vs natural foods. Brazil is in a state of deep industrialization meaning there is a boom in processed, and inexpensive food. Although China is in the same state, the culture tends to be more conservative with tradition and food. Therefore, China is more likely to eat traditional natural foods than Brazil (Kearney, 2010).
Additionally, the prevalence rates of ethnicities (Asians) within America versus their homeland counterparts are drastically different. There is a higher prevalence rate in America as well as several other developed countries when comparing the same ethnicities. This rules out genetics in this specific comparison which leaves the culture and lifestyle of each to be compared. The major difference between each country is the food habits in which American ethnic populations are more likely to be more westernized (including foods) than their motherland. (Figure 1)
Are there differences in the gut microbiome composition of diversity worldwide?
In an attempt to determine whether a geographical and gut-microbiome relationship impacts PD likelihood, it’s important to examine whether the gut-microbiome composition varies predictably across the globe. Even among a diverse country that shares similar features nationwide, yet has a relatively high diversity of ethnicities such as the United States of America, there seems to be a difference in the epidemiology among ethnicities. Although there are several control variables with a nationwide population, there are likely external factors that affect the rate of infection among specific ethnicities. In a study done by Willis et al., (2010) the team came to a conclusion that among Americans there is a higher rate of PD among Caucasians than the Asian or African demographic (Wright, Willis et al., 2010). Although genetics may seem to be a significant reason for this, experts claim only around 15% of Parkinson’s development is reliant on genetics (Johns Hopkins Editing, 2014). The other 85% may be related to factors of the environment, including food intake. Thus, the food that those in eastern countries eat is different from those found in western cuisine which could be a major factor in the difference in ethnicities within the same country. There seems to also be a tie between the geographic locations/diets of remote Indian villages and their Gut-bacteria profile (GBP). This exemplifies that there is observed data that the gut is being affected by the foods eaten as well as the location of tribes (Dehingia et al., 2015). Through this, we are able to suggest that diet will alter the gut, and consequently the brain.
Is there a correlation between PD and the Gut-brain axis?
As introduced above, the gut-brain axis includes the populations of organisms present in our gut, the gut microbiome, and its influence on the functioning of our nervous system. We were interested in determining whether there were components of this axis that were specific to those patients with PD. In a study done by Quigley (2017), germ-free mice (or those that lacked a microbiome) demonstrated decreased expression of the important neurotrophic factor, brain-derived neurotrophic factor (BDNF) in several brain areas including the cortex, hippocampus, and amygdala. Additionally, others have demonstrated impaired neurogenesis in the hippocampus and altered neural morphology in the amygdala in germ-free animals (Quigley, 2017). Through this study and several others, we can begin to see the link between the microbiome of the gut and the health and cognition of the brain. Thus, gut bacteria with immune activation go through a defective gut barrier, which eventually leads to a systemic inflammatory response which, consequently, impairs the blood-brain barrier and promotes neuroinflammation, and finally leads to neural injury and degeneration. This gives evidence for the influence of the gut-brain axis on all neural disorders.
Despite the many factors associated with PD, including aging and genetics, there is also a likely influence on the microbiota. In a study done by Romano et. al. (2021), they have found significant alterations between the microbiome of PD patients and control groups (Romano et al., 2021). This is depicted in Tables 1 and 2.
Lactobacilli are commonly found in yogurt which is a daily meal for south Asians. Typically they eat a small serving of homemade yogurt with each meal. Additionally, several eastern countries (African countries, Asian countries, etc.) use probiotic ingredients such as onions and garlic much more frequently than western countries. This may additionally explain the lower correlation of PD in Eastern countries than Western countries (Abbas et al., 2017). Although some articles disagree on certain levels of these bacteria, the majority agree with what is stated in this review. Additionally, it may vary due to location and diet.
Bacilli are a wide range of bacteria that are very helpful for improving digestion, immune modulation, and growth performance. They are very helpful for the overall health of our body. These bacteria can be found in numerous foods including vegetables and raw foods (Bernardeau et al., 2017). They can also be benefitted from the consumption of probiotics, similar to other bacteria. (Table 2)
Phascolarctobacterium is also another bacteria commonly found in the gut which has variations between PD patients and the control group. This bacteria has been known to help metabolic reactions and processes. It has also been found in higher amounts with a higher fiber intake (Cross et al., 2017). It has also been found to increase substantially in the gut from the use of Berberine and Metformin (Wu et al., 2017), which may be an area of future interest.
Akkermansia has been found to decrease the risk of heart disease, cholesterol issues, and fat storage. It has also been found to decrease inflammation, prevent weight gain, and improve immunity. This specific bacteria is obtained from fatty fish and Polyphenols. This has also been seen at increased levels in PD patients.
Ruminococcus torques has also been noticed to be increased in PD patients. This specific bacteria has been known to decrease the gut barrier integrity and is pro-inflammatory (Deaver et al., 2018). It also is known to help break down cellulose and resistant starches (Tomova et al., 2019). This bacteria is benefited by long-term fruit and vegetable consumption.
In addition to individual strains, gut microbiota diversity may be another factor influencing the risk for PD. In many PD patients, the diversity within the gut is lower than that of a control patient. In a study done by Li et al. titled “Gut Microbiota Differs Between Parkinson’s Disease Patients and Healthy Controls in Northeast China”, the authors took a group from Northeast China and derived a study from them using PD cases and control groups. From this study, they determined that there was a significant difference between the PD group and the control group in regards to their diversity (Li et al., 2019). The PD group had decreased species richness, β-diversity, phylogenetic diversity, and altered amount of taxa when compared to a control. Using data collected from the same article which provides which specific bacteria are altered between a PD patient and a control group in which this data can be interpreted. Additionally, it seems that due to the increased levels of other bacteria among the PD patients’ gut microbiome there may be a decrease in the diversity of PD patients. Since there are increased bacteria of several taxa and only a few decreased taxa the diversity is likely to decrease. The carrying capacity of bacteria in the gut does not get impacted whether or not one has PD, therefore when several taxa increase there is less space for less frequent taxa to thrive since they are being outcompeted due to the increased abundance of other taxa in PD patients.
Geographical and ethnic influence on gut microbiota and its impacts on PD prevalence
As a summary of what we present above, there seems to be a correlation between geographical location and PD prevalence. Although ethnic genetics may be one factor in its occurrence, a majority of the cause seems to be environmentally based. One such environmental factor includes the foods consumed and the resulting microbiome. Thus, the geographical location may influence one’s GBA which may lead to a risk of developing PD.
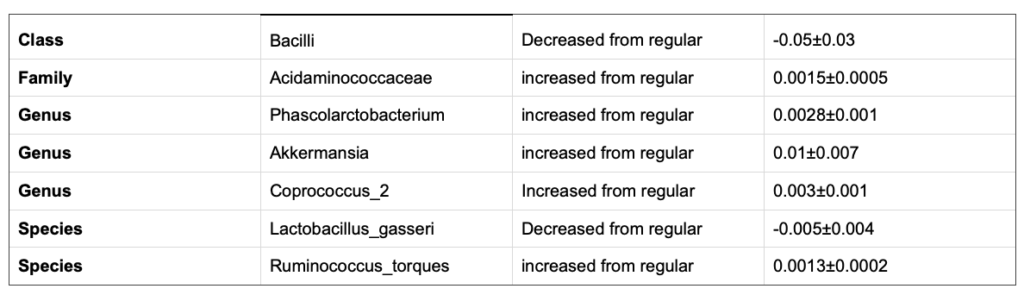
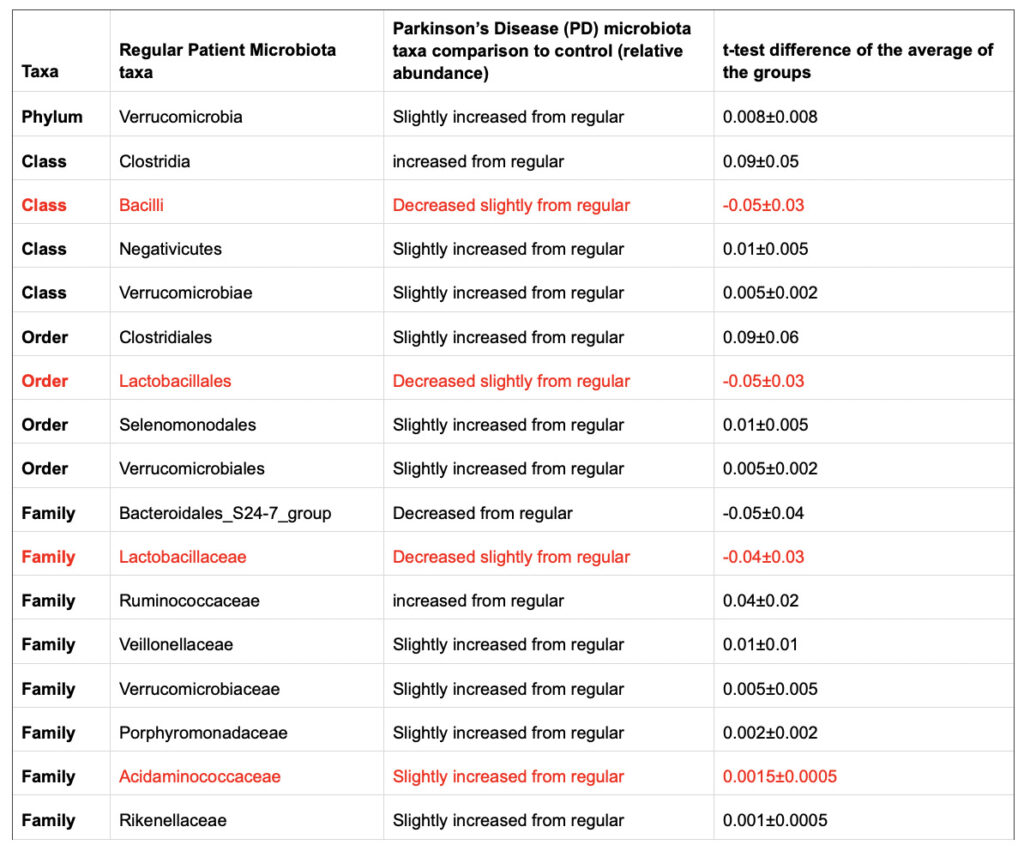
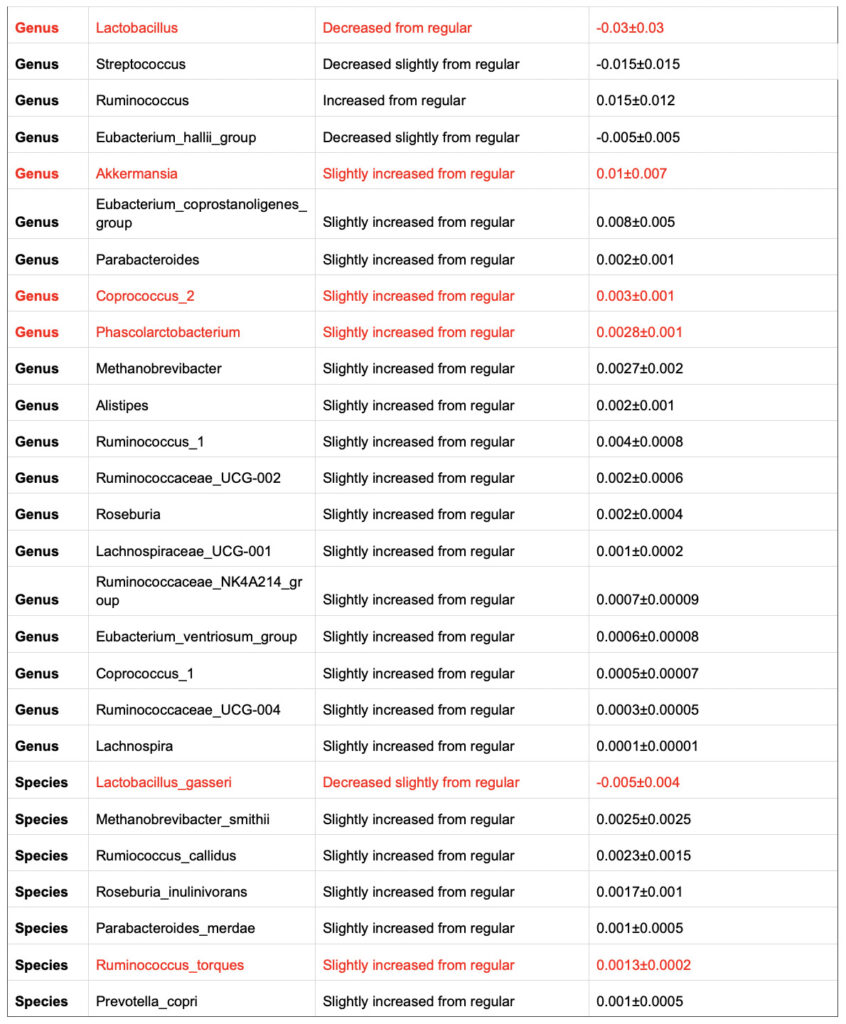

Table 1. Table focusing on the bacteria discussed in the text. *Obtained from Li et al. (2019)

Discussion:
Given the above data from the existing literature, we suggest a relationship between areas with a higher incidence of Parkinson’s, such as the western world (ie: America, South America, etc), and microbiome content. Specifically, the gut microbiomes of those with PD tend to contain lower levels of Lactobacillales, as well as a lower gut diversity. Beyond this, the results presented show patterns that are open to educated scientific interpretation and will be discussed further.
This novel study covers a large-scale review of Parkinson’s epidemiology in relation to ethnicity/geographical location with the gut-brain axis. From the results discussed above, it has been seen through several studies that there are ranging levels of prevalence rates of PD in different countries (Figure 1). Although a portion of this could be due to genetics, it is too large of a difference showing there are external factors influencing this. Specifically, these results demonstrate differences in the PD prevalence of the Eastern vs Western countries. As seen in Figure 1, the redder and orange coloring indicated areas in the western countries, although there is also orange found in some Eastern countries. This seems to correlate with rapidly industrializing cities. From this figure, we are able to suggest a cultural factor (food habits, traditions, etc.) that may enable the differences between the two hemispheres. Thus, this could be due to a difference in food consumption.
One type of food item consumed is one containing probiotics. Probiotics are always a welcomed food item into the body. Examples of this may be yogurt, buttermilk, kefir, tempeh, kimchi, miso, sauerkraut, etc (How to get more probiotics 2020). These food items are largely eaten in eastern countries which also have a lower PD prevalence rate. One may argue that there are high levels of PD in some parts of the eastern countries as seen through Figure 1. This is due to the fact that the red/orange points in the east are rapidly industrializing and in these rapidly industrializing cities processed foods are typically more common than traditional foods in traditional regions (Kearney, 2010). This is because it is more efficient and inexpensive than traditional cooking methods, and is supported by the Epidemiological transition model (ETM) typically the fifth stage (which includes developed countries such as the USA, Germany, Canada, etc.) are normally facing infectious diseases being replaced as the major cause of natural death by degenerative diseases (such as Parkinson’s). Using this model we can see that there has been repeated data collected which shows that degenerative diseases have been seen continuously to be prevalent in developed countries (McKeown, 2009). For this reason, it makes sense that rapidly developing cities would be redder than more traditional cities. An example of this in Figure 1 is within India; we see Bombay as highlighted in orange while Kalkutta (a more slowly developing city) is yellow.
We additionally believe there is a correlation between the prevalence of PD and processed foods, a trademark of western culture, through the results above. As mentioned above, traditional cities do not have as many processed foods while industrializing cities (which are redder in Figure 1) tend to have much more processed foods. Additionally, there have been studies done such as Leo et. al (2019) which demonstrates an impact on brain health in a highly-processed diet. They show that ultra-processed diets may lead to low-grade systemic inflammatory and oxidative changes. These factors are very incubative of neurodegenerative diseases such as Parkinson’s and Alzheimer’s. We believe our results collected along with the other studies done may strengthen this developing theory.
Food consumption directly impacts the content of the gut microbiome. We show a strong link between the gut-brain axis and the prevalence of PD. The health and diversity of the microbiome of the gut is likely a possible factor in the development of PD. There are specific genus/orders/families/species which are more probable to influence this specific neurodegenerative disease. We have also strengthened the line of reasoning between the variations of the gut microbiome worldwide and the variations of the gut microbiome between control and PD patients (Table 1 & 2).
This paper combines and builds upon existing research. This data is vital to understanding degenerative diseases due to the possibility of understanding which external factors influence them. Understanding a possible link between the factors presented here may help us begin to isolate which specific food causes the biggest impact and avoid them.
The generalizability of the results is limited by the lack of data collection of the epidemiology of PD and other factors worldwide. This includes data from those less developed countries and communities. The lack of this research makes it difficult to gauge what specific cultural differences make the largest impact. It also constricts the number of interpretations one can make about countries due to a large lack of resources. Specifically, there was a lack of data from several countries in Africa which made it difficult to discuss these regions in the results and discussion. Secondly, our understanding of the gut microbiota is still growing and evolving, so it is likely that we will learn more about the impact of specific strains in the future. Finally, future work may focus on the specific qualities of processed foods that may impact gut health in relation to the GBA. This could be hugely helpful in the overall goal of combatting PD as it can help to uncover the impact of these sources of food in developed and developing countries.
References
Abbas, M. M., Xu, Z., & Tan, L. C. S. (2017, December 22). Epidemiology of parkinson’s disease-east versus west. International Parkinson and Movement Disorder Society. https://movementdisorders.onlinelibrary.wiley.com/doi/full/10.1002/mdc3.12568.
Bernardeau, M., Lehtinen, M. J., Forssten, S. D., & Nurminen, P. (2017, July). Importance of the gastrointestinal life cycle of bacillus for probiotic functionality. Journal of food science and technology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5502041/#:~:text=In%20many%20animal% 20species%2C%20feed,feed%20processing%20and%20long%20storage.
Cross, T.-W. L., Zidon, T. M., Welly, R. J., Park, Y.-M., Britton, S. L., Koch, L. G., Rottinghaus, G. E., de Godoy, M. R. C., Padilla, J., Swanson, K. S., & Vieira-Potter, V. J. (2017, August 23). Soy improves Cardiometabolic health and Cecal microbiota in FEMALE Low-Fit RATS. Nature News. https://www.nature.com/articles/s41598-017-08965-0.
Deaver, J. A., Eum, S. Y., & Toborek, M. (2018, April 13). Circadian disruption changes gut microbiome taxa and functional gene composition. Frontiers. https://www.frontiersin.org/articles/10.3389/fmicb.2018.00737/full#:~:text=A%20metatranscriptomic %20analysis%20revealed%20an,layer%2C%20after%20circadian%20rhythm%20disruption.
Dehingia, M., Thangjam devi, K., Talukdar, N. C., Talukdar, R., Reddy, N., Mande, S. S., Deka, M., & Khan, M. R. (2015, December 22). Gut bacterial diversity of the tribes of India and comparison with the worldwide data. Nature News. https://www.nature.com/articles/srep18563?fbclid=IwAR243T7nvsdeadVZ6TPyuNZdb_BxV8CUu7BHS-9bEbul_UvnxD8TGV53JMs#Abs1.
GMFH Editing Team GMFH Editing Team. (2020, December 3). Get to know the Lactobacilli family. Gut Microbiota for Health. https://www.gutmicrobiotaforhealth.com/new-infographic-to-meet-lactobacilli/.
How to get more probiotics. Harvard Health. (2020, August 24). https://www.health.harvard.edu/staying-healthy/how-to-get-more-probiotics.
Johns Hopkins Editing. (2014). The genetic link to parkinson’s disease. Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/conditions-and-diseases/parkinsons-disease/the-genetic-link-to-parkinsons-disease#:~:text=About%2015%20percent%20of%20people,SNCA%20gene%20(see%20below).
Kearney, J. (2010, September 27). Food consumption trends and drivers. Philosophical transactions of the Royal Society of London. Series B, Biological sciences. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2935122/.
Li, C., Cui, L., Yang, Y., Miao, J., Zhao, X., Zhang, J., Cui, G., & Zhang, Y. (2019, July 11). Gut microbiota differs Between Parkinson’s disease patients and healthy controls in Northeast China. Frontiers in molecular neuroscience. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6637281/.
Mayo Foundation for Medical Education and Research. (2020, December 8). Parkinson’s disease. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/parkinsons-disease/symptoms-causes/syc-20376055?utm_source=Google&utm_medium=abstract&utm_content=Parkinsons-disease&utm_campaign=Knowledge-panel.
McKeown, R. E. (2009, July 1). The epidemiologic transition: Changing patterns of mortality and population dynamics. American journal of lifestyle medicine. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2805833/.
Quigley, E. M. M. (2017, October 17). Microbiota-Brain-Gut axis and neurodegenerative diseases. Current Neurology and Neuroscience Reports. https://link.springer.com/article/10.1007/s11910-017-0802-6.
Romano, S., Savva, G. M., Bedarf, J. R., Charles, I. G., Hildebrand, F., & Narbad, A. (2021, March 10). Meta-analysis of the parkinson’s disease gut microbiome suggests alterations linked to intestinal inflammation. Nature News. https://www.nature.com/articles/s41531-021-00156-z.
Tomova, A., Bukovsky, I., Rembert, E., Yonas, W., Alwarith, J., Barnard, N. D., & Kahleova, H. (2019, April 17). The effects of vegetarian and vegan diets on gut microbiota. Frontiers. https://www.frontiersin.org/articles/10.3389/fnut.2019.00047/full#:~:text=Ruminococcus%20is %20the%20third%20major,plant%20based%20foods%20(51).
WebMD. (2020). LACTOBACILLUS: Overview, Uses, side Effects, precautions, Interactions, dosing and reviews. WebMD. https://www.webmd.com/vitamins/ai/ingredientmono-790/lactobacillus.
What is parkinson’s? Parkinson’s Foundation. (2021). https://www.parkinson.org/understanding-parkinsons/what-is-parkinsons.
Wright Willis, A., Evanoff, B. A., Lian, M., Criswell, S. R., & Racette, B. A. (2010, January 15). Geographic and ethnic variation in PARKINSON disease: A population-based study of US Medicare beneficiaries. Neuroepidemiology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2865395/.
Wu, F., Guo, X., Zhang, J., Zhang, M., Ou, Z., & Peng, Y. (2017, October). Phascolarctobacterium faecium abundant colonization in human gastrointestinal tract. Experimental and therapeutic medicine. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5585883/.
About the author

Samay Inampudi
Samay is a Senior at Oswego East High School who loves socializing and the sciences. He loves life and lab sciences due to their complexity and precision. He participates in Science Olympiad, Ecology Club, and Model UN. Aside from his academic interests, he loves to spend time with his friends and plays tennis.